Testing for STIs at home? Yes, it’s possible—and popular
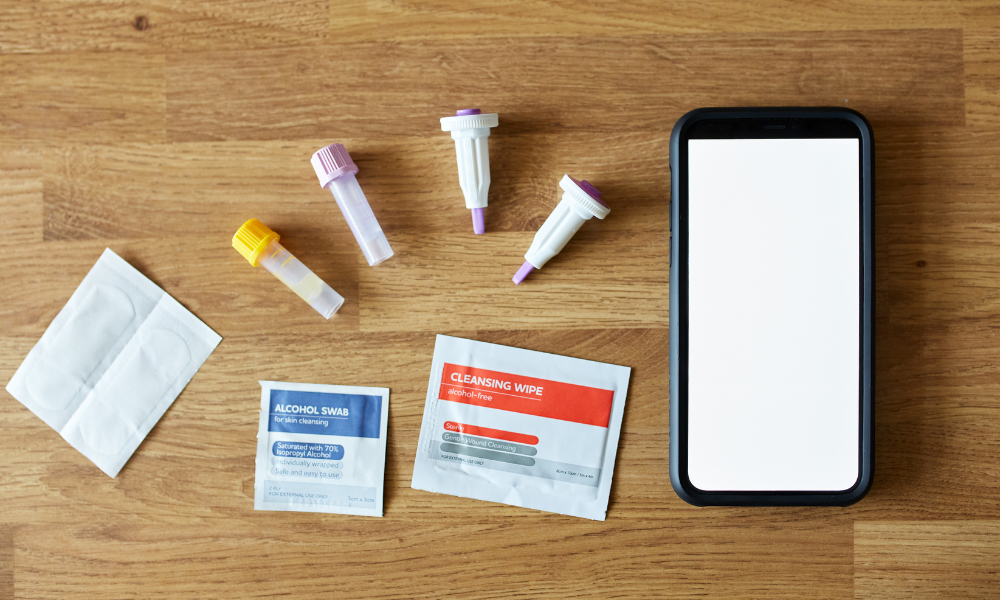
Testing for STIs at home? It’s possible, and an increasingly popular option. Read on to better understand how home testing works and what free at-home tests are available in your area.
Herpes—Fast facts

Herpes:Fast Facts Herpes is a common and usually mild infection caused by the herpes simplex virus (HSV). It can cause cold sores on the mouth or face (called oral herpes) as well as symptoms around the genitals, butt and thighs (called genital herpes). There are two types of HSV: herpes simplex virus type 1 (HSV-1) […]
Shortage of Only Eye Ointment to Protect Newborns from Gonorrhea-related Eye Infections Requires Alternative Options

There is a shortage of the only eye ointment to protect newborns from potentially serious eye infection that can be caused by chlamydia, gonorrhea, or other bacteria transmitted from parent-to-infant during birth.
Oklahoma Bill Would Criminalize STIs

The Oklahoma House recently passed a bill making it a crime to intentionally or recklessly spread several STIs. Those found guilty would be convicted of a felony and punished with between two and five years in prison.
Mpox Cases Almost Double from Last Year — Experts Worry Too Few People Are Vaccinated

Mpox cases in the United States are almost double what they were at this time last year. While rates still remain far lower than during the outbreak of 2022, experts worry too few people are vaccinated.
Diagnosing and Managing Genital Herpes: A Two-part Conversation with Terri Warren, RN, ANP

Diagnosing and Managing Genital Herpes A two-part conversation with Terri Warren, RN, ANP In this two-part episode of ASHA’s Sex+Health podcast, Terri Warren, RN, ANP—nurse, author, and owner of Westover Heights Clinic in Portland, Oregon that specializes in the genital herpes infection—explains the tests that can provide an accurate genital herpes diagnosis and how they […]
Doxy-PEP is a New Strategy to Help Prevent STIs

Doxy-PEP is the strategy of taking the antibiotic doxycycline after condomless oral or anal sex to prevent chlamydia, gonorrhea, or syphilis.
New Studies Add to Evidence that Doxy-PEP Works for STI Prevention

New studies add to our evidence that Doxy-PEP is working to prevent bacterial STIs among transgender women and men who have sex with men.
March is Sexual Pleasure Month—Celebrate it with Us!

March is Sexual Pleasure MonthCelebrate it with Us! Sex is good for you! Our bodies thrive on the chemicals released during orgasm, so a healthy sex life is part of a healthy body. We need to think of sexual health beyond the mere absence of disease: sexual pleasure and satisfaction are essential to our wellbeing. […]
Syphilis and Pregnancy — Preventing Congenital Syphilis

Congenital Syphilis A preventable problem The number of babies born with syphilis in the United States is increasing at an alarming rate. There were over 10 times as many babies born with syphilis in 2022 than in 2012. 0 infants born with syphilis in 2022 Syphilis during pregnancy can lead to miscarriage or stillbirth, and […]
Understanding Syphilis and How to Prevent It

Syphilis can be treated more easily if it is caught early. But undiagnosed and untreated syphilis can be dangerous. It can cause irreversible health damage and even death.
Do You Have to Be Turned on to Have Sex?

The number one complaint of women that I see for sexuality counseling is that they have no libido – zip, gone, disappeared. Contrary to what many of us assume, this happens to women of all ages and levels of love, attachment, and attraction to their partners.
