
HPV Screening with Self Collection Endorsed by Three Organizations
Three organizations—ACS, ACOG, and HRSA—have each recently endorsed new guidelines for cervical cancer screening. All of them discuss screening with self collected samples.

Unfortunately, there are many myths and misconceptions about genital HPV, and in some cases these can cause real harm. Bad information can cause a person to suffer terrible anxiety unnecessarily, to doubt a partner’s faithfulness, or even to undergo painful and expensive treatment that could have been avoided. Most dangerous of all, misinformation may lead people to neglect a very simple procedure that saves lives.
But why? One reality is that some aspects of the virus are still poorly understood, even by medical researchers. At the same time, much new information about HPV has been learned in recent years. The result is that older publications may be inaccurate. Likewise, health care professionals, writers, and educators who have not kept up with recent research findings may continue to spread misconceptions.
Another difficulty is that the overall topic of genital HPV is complex and confusing to everyone, lay person and scientist alike.
Below we take on some of the most common myths and misconceptions we’ve encountered on the topic of genital HPV and offer clear and accurate information in response.
Myth: “I’m the only person I know with HPV”
Fact: HPV is common. While many people diagnosed with HPV think they are alone, that’s far from the truth! It’s estimated that more than 80% of sexually active people will have HPV at some point in their lives. Since most often genital HPV produces no symptoms or illness, and so a person who has been infected may never know about it.
Myth: Only people who have casual sex get sexually transmitted infections (STIs).
Fact: Anyone who is sexually active can get an STI, like HPV. Even though nearly 20 million Americans will get a sexually transmitted infection (STI) each year, many people still believe that only “other people”—for example, people who have multiple partners, sex outside of marriage, or a different lifestyle—can contract one.
It is true that a higher number of sexual partners over the course of a lifetime does mean more opportunities to be exposed to an STI, including HPV. This is not because of any moral judgment concerning “casual” sex as compared with “committed” sex, but simply because the more sexual partners you have, the more likely you will have a partner who (knowingly or unknowingly) is carrying an STI. STIs can be passed along as readily in a loving, long-term relationship as in a one-night stand.
Myth: An HPV diagnosis means someone has cheated.
Fact: Even after an HPV infection is diagnosed, there is simply no way to find out how long a particular infection has been in place, or to trace it back to a particular partner.
The virus can remain in the body for weeks, years, or even a lifetime, giving no sign of its presence. Or a genital HPV infection may produce warts, lesions, or cervical abnormalities after a latent period of months or even years. This is one of the most mysterious aspects of genital HPV: its ability to lie latent (or “asleep”).
This myth has been responsible for a great deal of anger, confusion, and heartache. It has led many people to tragically wrong conclusions. As mentioned above, most people who are infected with genital HPV never know it. In most cases, a person is diagnosed with HPV only because some troubling symptom drove him or her to a health care professional, or some abnormality was revealed in the course of a routine exam.
In a monogamous relationship, therefore, just as in an affair or even in an interval of no sexual relationships at all, an HPV diagnosis means only that the person contracted an HPV infection at some point in his or her life.
Myth: Genital warts lead to cervical cancer.
Fact: The fleshy growths we call genital warts are almost always benign. The Centers for Disease Control and Prevention states it clearly: “No evidence indicates that the presence of genital warts or their treatment is associated with the development of cervical cancer.”
As for ordinary genital warts, says Doug Lowy, MD, chief of the Laboratory of Cellular Oncology at the National Cancer Institute, “These are caused by HPV types that are virtually never found in cancer.” These are the “low-risk” types, 6, 11, 42, 43, and 44. When not causing genital warts they may cause a transient abnormality in Pap test results, or most often produce no symptoms at all.
It is worth keeping in mind that both men and women may be infected with, and infectious for, cancer-causing types of HPV, regardless of whether or not they have genital warts.
Myth: An abnormal Pap test means cervical cancer.
Fact: Most people with an abnormal Pap will never develop cancer. First of all, an abnormal Pap test can be caused by factors other than the presence of a high-risk HPV type. When a Pap test comes back as “abnormal,” it means just that. Under the microscope, the appearance of a few cells in this sample differs in some way from the classic appearance of healthy, intact cervical cells. The difference could be due to local irritation, a non-HPV infection, a non-cancer-causing HPV type, or even a mistake in the preparation of the cell sample.
To help sort out the various possibilities, a woman with an abnormal Pap test will likely have follow up testing. A Pap is a screening test, not a diagnostic one, so a provider will help determine the next steps to take, which may include additional testing or procedures such as colposcopy and biopsy.
But this very effective system of protection can work only when women get screened regular intervals. More than 50% of all new cervical cancers are in women who have never been screened or have been infrequently screened.
Myth: If I have HPV, I will have recurrences.
Fact: Warts and dysplasia do come back in some cases, but by no means all. When they come back, they show varying persistence: Some people have just one more episode, and others several. The good news for most people is that with time, the immune system seems to take charge of the virus, making recurrences less frequent and often eliminating them entirely within about two years.
The limiting factor here is the state of the immune system itself. According to Thomas Sedlacek, MD, adjunct professor of obstetrics and gynecology at Allegheny University, if an individual’s immune system is impaired—by the use of certain medications, by HIV infection, or by some temporary trauma such as excessive stress, serious illness, or surgery—it may be unable to prevent a recurrence. However, if the immune system is weakened only temporarily, most likely the recurrence will be brief.
The concern about life-long recurrences may be based on a misconception rather than a myth. It’s true that at present there is no known cure for genital HPV. As a virus, it will remain in the infected person’s cells for an indefinite time—most often in a latent state but occasionally producing symptoms or disease. Recent studies from the Albert Einstein College of Medicine and from the University of Washington suggest that HPV may eventually be cleared in most people with well-functioning immune systems. However, in at least some cases the virus apparently does remain in the body indefinitely, able to produce symptoms if the immune system weakens.
Myth: Lesbians don’t need regular cervical cancer screening.
Fact: HPV screening is recommended for gay and straight women alike. This myth is based on an overly simple view of how HPV can be transmitted. Yes, penile-vaginal sex can pass the virus along from one partner to another, but HPV can be passed through other forms of skin-to-skin contact as well.
Evidence for this comes from a study at the University of Washington, which found a number of genital HPV infections among lesbians—even in some women who had never had sex with a man. Newer research confirms that HPV is common among women with same-sex partners. Regular screening is essential prevention for all women regardless of sexual orientation.
Myth: If a woman has an abnormal Pap, her male partner needs to be tested for HPV.
Fact: There is no diagnostic test that can accurately determine whether a man is carrying an HPV infection. And even if he does, there is no way to treat him for the virus.
According to recent guidelines drafted by the CDC, “examination of sex partners is not necessary” as follow-up to an abnormal Pap test. It’s certainly possible—even likely—that the partner is or has been infected with the virus, although highly unlikely that he will ever show any symptoms. Nor is it possible to determine whether he can spread HPV to a future partner.
However, if a woman has external genital warts, her partner may still consider scheduling a medical exam. It may be useful for a male partner to talk with a health care provider to gain more information. And of course, if a man starts to notice symptoms of his own, such as unexplained bumps or lesions in his genital area, he should get medical attention at once.
Myth: If I’ve always used condoms, I’m not at risk for HPV.
Fact: Used correctly, condoms are very effective against STIs such as chlamydia, gonorrhea, and HIV that are spread through bodily fluids. However, they are likely to be less protective against STIs that spread through skin-to-skin contact, such as HPV and herpes. The reason is simply that condoms do not cover the entire genital area of either sex. They leave the vulva, anus, perineal area, base of the penis, and scrotum uncovered, and contact between these areas can transmit HPV.
That is not to say condoms are useless. In fact, studies have shown condom use can protect against HPV infection and HPV-related diseases, as well as help prevent other STIs and unintended pregnancy.
Adapted from “10 Myths About HPV” by Sandra Ackerman. Reprinted from HPV News (c) The American Sexual Health Association

Three organizations—ACS, ACOG, and HRSA—have each recently endorsed new guidelines for cervical cancer screening. All of them discuss screening with self collected samples.
Research suggests that only one dose of the HPV vaccine may be effective enough to prevent HPV-related disease, including cancer.

Australia has been a leader in cervical cancer prevention for decades and is now close to eliminating the disease.

The American Cancer Society (ACS) released new recommendations for cervical cancer screening that focus on HPV testing and approve the use of self-collected samples. The recommendations also clarify the age at which screening should start and stop.
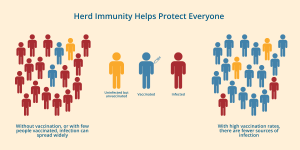
We’ve known for years that the HPV vaccine works. Now new research shows that widespread vaccination even protects those who haven’t gotten the shot. This study proves that it is possible to reach herd immunity for HPV.

HPV is one of the most common sexually transmitted infections. Still, finding out that you or your partner has it can feel stressful and confusing. It’s normal to have a lot of questions: What does this mean for our health? Did someone cheat? Should we

The FDA just approved the Teal Wand, a self-collection device for HPV testing that does not require a speculum exam or even a trip to the doctor’s office. People can collect their own sample at home and send it to a lab for analysis.

The results of large-scale study of HPV suggest that one shot of the vaccine may be enough to protect young people from HPV and related issues like cervical cancer.
ASHA believes that all people have the right to the information and services that will help them to have optimum sexual health. We envision a time when stigma is no longer associated with sexual health and our nation is united in its belief that sexuality is a normal, healthy, and positive aspect of human life.
ABOUT
GET INVOLVED
ASHA WEBSITES
GET HELP
© 2026 American Sexual Health Association
We need to know if we can keep you company during this visit. We are useful for making this site work.
We use cookies to enhance your browsing experience. You can choose which cookies you want to accept.
Necessary cookies help make a website usable by enabling basic functions like page navigation and access to secure areas. The website cannot function properly without these cookies.
| Cookie | Provider | Purpose | Expiry |
|---|---|---|---|
digiconsent | This website | Stores your cookie consent preferences. | 1 year |
wordpress_logged_in_* | WordPress | Identifies logged-in users and their authentication details. | 14 days / Session |
wordpress_sec_* | WordPress | Stores authentication details for secure areas. | 14 days / Session |
wp-settings-* | WordPress | Stores user interface customization preferences. | 1 year |
wp-settings-time-* | WordPress | Stores the time when wp-settings cookie was set. | 1 year |
Analytics cookies help us understand how visitors interact with our website by collecting and reporting information anonymously. This helps us improve our website.
| Cookie | Provider | Purpose | Expiry |
|---|---|---|---|
_ga | Registers a unique ID to generate statistical data on website usage. | 2 years | |
_ga_* | Used by Google Analytics to store and count pageviews. | 2 years |
Marketing cookies are used to track visitors across websites. The intention is to display ads that are relevant and engaging for the individual user.
Functional cookies enable the website to provide enhanced functionality and personalization. They may be set by us or by third party providers.