
Fewer Women Are Getting Prenatal Care (and Missing an Important Chance to Prevent Congenital Syphilis)
A new report shows that fewer women are getting prenatal care. That means too many patients are missing the chance to prevent congenital syphilis.

Syphilis is a bacterial infection, caused by the bacteria Treponema pallidum. It is passed on when a person comes in contact with a syphilitic sore, known as a chancre—typically during vaginal, anal, or oral sex. Syphilis can also be passed on during pregnancy or childbirth from a pregnant person to their baby.
Syphilis can be treated more easily if it is caught early. But undiagnosed and untreated syphilis can be dangerous. It can cause irreversible health damage and even death.
At this moment, syphilis cases are increasing and there is a surge in cases of cases among newborns, called congenital syphilis. Over 10 times as many babies were born with syphilis in 2022 than in 2012. Syphilis during pregnancy is a serious issue. It can cause miscarriage, stillbirth, and even infant death. Babies born with syphilis can face lifelong medical issues. This is why testing for syphilis is recommended for all pregnant patients, so infections can be found and treated.
With reported cases of syphilis up 80% since 2018 and more than 3,700 babies born with syphilis in 2022, it’s important to learn more about this curable STI and how to protect yourself from serious health consequences.
According to the Centers for Disease Control and Prevention (CDC), there were more than 207,255 cases of syphilis in 2022. Most cases of syphilis reported in the United States are in men, with the majority cases in gay, bisexual, and other men who have sex with men (MSM). However, there has been a rise in cases of syphilis in infants—called congenital syphilis—in recent years.
Sexually
Non-sexually
If left untreated, syphilis can move to the secondary stage. This stage of syphilis can develop 17 days to 6 1/2 months after infection and symptoms can last from 2 to 6 weeks.
Symptoms in this stage include a rough, reddish-brown rash or spots on the palms of hands, soles of feet, or rashes on other parts of the body, including the neck, head and torso. Other symptoms could include headache, fever, and generally not feeling well.
The symptoms will go away on their own, but the disease will still be present if untreated. It will then enter into a latent stage, which has no signs or symptoms.
The latent stage begins when the primary and secondary stage symptoms are gone and the infection has been left untreated. During this stage, which can last for as long as 20 years, there are no symptoms, but syphilis is still there.
Symptoms of late stage (also called tertiary syphilis) can occur 2 to 20+ years after infection.
Untreated syphilis can result in damage to organs, including the brain, eyes, heart, bones and joints. The damage caused by untreated syphilis can even lead to death.
Syphilis can be detected by blood tests, which looks for antibodies, or by testing fluid taken from lesions or swollen lymph nodes, which occur during primary or secondary syphilis. Tests on the lymphatic fluid or lesions look for antigens.
Blood tests can be done in all stages of syphilis. There are two types of blood tests available for syphilis—both types are needed to confirm that a person has syphilis.
This is the definitive method for diagnosing early syphilis and congenital syphilis. This test uses a fluid sample taken from the chancre (sore) during primary syphilis or from symptoms that occur during secondary syphilis found in areas such as the vagina or the urethra. The sample is then viewed under a microscope.
If no signs and symptoms are found at birth, a blood test should be performed every 2 to 3 months on the infant until the test comes back negative. This is because an infant may test positive for syphilis and not be infected until the mother’s antibodies, transmitted during pregnancy, clear the infant’s body.
Left untreated, syphilis can cause blindness, paralysis, and problems with your bones and internal organs, including your heart.
Telling a partner can be hard, but keep in mind that some people with syphilis don’t know they have it. It’s important that you talk to your partner as soon as possible so they can get treatment. Also, it is possible to pass syphilis back and forth, so if you get treated and your partner doesn’t, you may get infected again.
Congenital syphilis is a public health crisis. You can help raise awareness about the striking rise in syphilis with our social media toolkit. Share our images and messages on all of your social channels—just click to download and copy/paste.

A new report shows that fewer women are getting prenatal care. That means too many patients are missing the chance to prevent congenital syphilis.
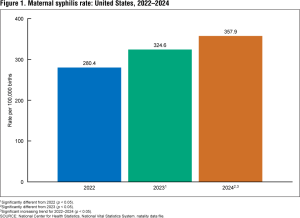
Syphilis rates in pregnant women went up 222% percent between 2016 and 2022 and another 28% between 2022 and 2024. Too many pregnant women are not being screened.

A new study found that opt-out screenings for all patients in emergency departments caught numerous cases of syphilis and HIV that would have gone undetected under other screening protocols.

According to the Great Plains Tribal Epidemiology Center, syphilis rates among Native Americans in Iowa, Nebraska, North Dakota, and South rose 1,865% from 2020 to 2022.
The FDA recently approved an at-home test for syphilis that can provide initial results in just 15-minutes. Syphilis has been surging in recent years with the number of cases rising 80% between 2018 and 2022 alone.
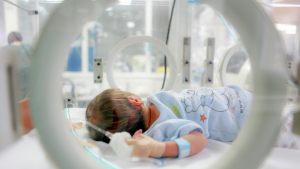
Public health experts have said that every case of congenital syphilis is a failure of STI screening and prenatal care. A new study looked more closely at cases to see what factors in a pregnant person’s life were most associated with congenital syphilis.
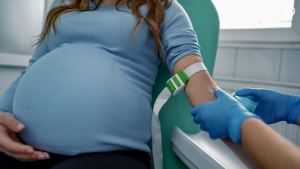
The American College of Obstetricians and Gynecologists released new guidelines recommending that all pregnant people be screened for syphilis three times during pregnancy.

New studies add to our evidence that doxy PEP works to prevent bacterial STIs among transgender women and men who have sex with men.
ASHA believes that all people have the right to the information and services that will help them to have optimum sexual health. We envision a time when stigma is no longer associated with sexual health and our nation is united in its belief that sexuality is a normal, healthy, and positive aspect of human life.
ABOUT
GET INVOLVED
ASHA WEBSITES
GET HELP
© 2026 American Sexual Health Association
We need to know if we can keep you company during this visit. We are useful for making this site work.
We use cookies to enhance your browsing experience. You can choose which cookies you want to accept.
Necessary cookies help make a website usable by enabling basic functions like page navigation and access to secure areas. The website cannot function properly without these cookies.
| Cookie | Provider | Purpose | Expiry |
|---|---|---|---|
digiconsent | This website | Stores your cookie consent preferences. | 1 year |
wordpress_logged_in_* | WordPress | Identifies logged-in users and their authentication details. | 14 days / Session |
wordpress_sec_* | WordPress | Stores authentication details for secure areas. | 14 days / Session |
wp-settings-* | WordPress | Stores user interface customization preferences. | 1 year |
wp-settings-time-* | WordPress | Stores the time when wp-settings cookie was set. | 1 year |
Analytics cookies help us understand how visitors interact with our website by collecting and reporting information anonymously. This helps us improve our website.
| Cookie | Provider | Purpose | Expiry |
|---|---|---|---|
_ga | Registers a unique ID to generate statistical data on website usage. | 2 years | |
_ga_* | Used by Google Analytics to store and count pageviews. | 2 years |
Marketing cookies are used to track visitors across websites. The intention is to display ads that are relevant and engaging for the individual user.
Functional cookies enable the website to provide enhanced functionality and personalization. They may be set by us or by third party providers.