
Is Doxy PEP Responsible for a Drop in STI Rates in San Francisco?
New data shows that cases of bacterial STIs have dropped dramatically in San Francisco. Public health officials in the city believe doxy PEP has helped drive these declines.

Mpox cases in the United States are almost double what they were at this time last year, according to new data from the Centers for Disease Control and Prevention (CDC). While rates still remain far lower than they were during the outbreak of 2022, experts worry that too few people are vaccinated.
As of mid-March, there were an estimated 511 cases of the virus compared to just 287 at the same time last year. New York City has had over 100 cases so far this year compared to just 30 last year, and the Virginia Department of Health recently issued a warning about a rise in cases in the state.
Dr. Brandy Darby, director of the department’s Division of Surveillance and Investigation told CNN: “We felt like it was really important to get the word out that there is a continued risk from this virus. It’s still here.”
Mpox, which used to be known as monkeypox, is a virus that causes flu-like symptoms and a rash/sores on the skin. It is transmitted through skin-to-skin contact or contact with an infected person’s clothing, towels, or bedding. While not technically an STI, mpox is passed through close physical contact.
The majority of the cases in the 2022 outbreak were the result of sexual behavior. Anyone can get mpox, but gay and bisexual men, other men who have sex with men, and transgender individuals were disproportionately affected by that outbreak.
A survey from August of that year found that about half of men who have sex with men changed their behaviors during the mpox outbreak. Many chose to have fewer sex partners, use dating apps less frequently, and/or have fewer one-time sexual encounters. Research has found that these changes did a lot to curb the spread of mpox. While this was important during the outbreak, it is not sustainable or necessary long term.
Instead, the CDC recommends the JYNNEOS vaccine for people who are likely to be exposed to mpox, including gay, bisexual, and other men who have sex with men or are transgender, gender non-binary, or gender-diverse. Specifically, the agency suggests the vaccine for members of this community who, in the last six months, have had more than one partner, been diagnosed with an STI, visited commercial sex venues (like sex clubs or parties), or had sex at a large public event (like a festival) in areas where mpox transmission is occurring. Partners of people who fit these criteria should also get vaccinated. The vaccine is also recommended for anyone who has HIV or other immune system issues.
The vaccine is given in two doses. Vaccination rates are still not what they should be, however. In most states less than a quarter of the population at risk has been fully vaccinated, and coverage is below 10% in eight states.
As rates of mpox go up, the CDC is recommending that anyone who fits the criteria and has not been fully vaccinated do so now. Ideally, doses are given four weeks apart, but experts are suggesting that anyone who has had one dose get the second one as soon as possible regardless of when the first was given. There is no supply issue so vaccines should be readily available. The mpox vaccine locator below can help people find vaccines in their area.

New data shows that cases of bacterial STIs have dropped dramatically in San Francisco. Public health officials in the city believe doxy PEP has helped drive these declines.

A new report shows that fewer women are getting prenatal care. That means too many patients are missing the chance to prevent congenital syphilis.

Condoms. All sorts of shapes, sizes, colors (even glow-in-the-dark). Ribbed or plain. Lubed or not. Latex or plastic. ASHA’s Fred Wyand shares his thoughts on this reliable way to prevent STIs and pregnancy.
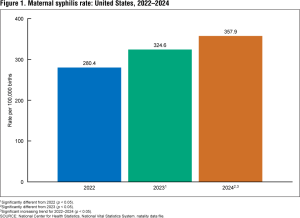
Syphilis rates in pregnant women went up 222% percent between 2016 and 2022 and another 28% between 2022 and 2024. Too many pregnant women are not being screened.

Three organizations—ACS, ACOG, and HRSA—have each recently endorsed new guidelines for cervical cancer screening. All of them discuss screening with self collected samples.
Research suggests that only one dose of the HPV vaccine may be effective enough to prevent HPV-related disease, including cancer.
ASHA believes that all people have the right to the information and services that will help them to have optimum sexual health. We envision a time when stigma is no longer associated with sexual health and our nation is united in its belief that sexuality is a normal, healthy, and positive aspect of human life.
ABOUT
GET INVOLVED
ASHA WEBSITES
GET HELP
© 2026 American Sexual Health Association
We need to know if we can keep you company during this visit. We are useful for making this site work.
We use cookies to enhance your browsing experience. You can choose which cookies you want to accept.
Necessary cookies help make a website usable by enabling basic functions like page navigation and access to secure areas. The website cannot function properly without these cookies.
| Cookie | Provider | Purpose | Expiry |
|---|---|---|---|
digiconsent | This website | Stores your cookie consent preferences. | 1 year |
wordpress_logged_in_* | WordPress | Identifies logged-in users and their authentication details. | 14 days / Session |
wordpress_sec_* | WordPress | Stores authentication details for secure areas. | 14 days / Session |
wp-settings-* | WordPress | Stores user interface customization preferences. | 1 year |
wp-settings-time-* | WordPress | Stores the time when wp-settings cookie was set. | 1 year |
Analytics cookies help us understand how visitors interact with our website by collecting and reporting information anonymously. This helps us improve our website.
| Cookie | Provider | Purpose | Expiry |
|---|---|---|---|
_ga | Registers a unique ID to generate statistical data on website usage. | 2 years | |
_ga_* | Used by Google Analytics to store and count pageviews. | 2 years |
Marketing cookies are used to track visitors across websites. The intention is to display ads that are relevant and engaging for the individual user.
Functional cookies enable the website to provide enhanced functionality and personalization. They may be set by us or by third party providers.