
HPV Screening with Self Collection Endorsed by Three Organizations
Three organizations—ACS, ACOG, and HRSA—have each recently endorsed new guidelines for cervical cancer screening. All of them discuss screening with self collected samples.
Dr. Joel Palefsky is an expert in infectious diseases and cancers associated with these diseases. He is an internationally recognized expert in human papillomavirus (HPV) infections of the anus and genitals and specializes in people living with HIV. He recently led the Anal Cancer/HSIL Outcomes Research (ANCHOR) Study, a multi-site study that examined whether detecting and treating pre-cancerous lesions could prevent anal cancer.
Dr. Palefsky is the founder and president of the International Anal Neoplasia Society as well as the founder and chairperson of the International Papillomavirus Society’s global campaign for HPV awareness.
ASHA recently sat down with Dr. Palefsky to talk about HPV and anal cancer.
Anal cancer is very similar to cervical cancer and is caused by the same HPV types. It’s still a pretty rare disease but incidence has been increasing since the 1970s.
It is more common in women than men in the general population, but there are certain groups that are known to be especially high risk. Those include people with HIV and women with a history of vulvar cancer and cervical cancer. Men who have sex with men—particularly HIV-positive MSM—are the highest risk group.
Not always. About half of the women in many of the studies that have been done had never had anal sex. These people are presumably getting HPV of the anus from infections of the cervix or vulva. The other half have had anal sex, which is a common sexual practice.
This is probably one of the reasons why anal cancer is more common in women than men because women have more opportunities to get HPV. But, again, those who have more anal sex, namely the MSM, do have a much higher risk of anal cancer. When you throw HIV on top of that, it raises the risk even more.
Because there’s no screening for it, most people don’t seek help until they present with symptoms—usually bleeding, pain, or a mass that they can feel. The typical story for someone who isn’t known to be at risk is that they go see their doctor for rectal bleeding and are told they have hemorrhoids. Sometimes they even get surgery hemorrhoids and when the pathology comes back, they find out it is cancer.
There are screening tests that are similar to those we use for cervical cancer. We can swab the area and screen for precancerous changes with cytology, and we can also sometimes test for HPV.
There is also a procedure called High Resolution Anoscopy or HRA in which we examine the anal canal with a high-resolution instrument called a colposcope. We visualize the whole anus using the same sort of stain we use in the cervix—acetic acid—and take biopsies to see if they have anal precancer [called high-grade squamous intraepithelial lesions] and rule out cancer.
If the biopsies come back showing these, we repeat the procedure but this time the approach is usually to use electrocautery. We use a version called hyfrecation in which we try to remove the affected area but lose as little of the normal tissue as possible. It’s done in the office and is quick, 20-minute procedure that’s very well tolerated and not painful.
The ANCHOR study included nearly 4,500 participants with HIV. It was not a screening study because one of the key entrance criteria was biopsy-proven, high-grade disease [anal pre-cancer]. We did HRA on everybody in the study because it’s the gold standard diagnostic procedure. And as it turns out, that was a good thing to have done because what we found was an extraordinarily high prevalence of these high-grade lesions. About half the population had these high-grade changes.
The real goal of the study was to show that we could significantly reduce the incidence of anal cancer by treating pre-cancer and we did this even before we finished recruiting for the study. It was a randomized controlled trial; half the people were treated and half were untreated.
We’ve been following up to make sure that the people who had not been treatment were offered the opportunity to get treated and to continue following the people we’d treated before. All clinical follow up just ended.
The CDC is about to release guidelines on anal cancer screening using cytology and HRA. These are mostly limited to people with HIV because that’s where the research has been done. There are other guidelines recently published in the International Journal of Cancer which add some other high-risk groups to those who should get screened this way.
We’re not recommending that everyone be screened this way because anal cancer is rare. The risk for the general population is just too low. But our next step should be to ramp up infrastructure so more places have providers who can do HRA. Right now it’s concentrated in cities with large MSM populations but there are many communities in the United States where no one knows how to do this.
We do recommend that everyone get a digital anal rectal exam. We call that a DARE. People are more familiar with digital rectal exams [in which a health care provider inserts a gloved finger into the anus/rectum]. These are primarily aimed at finding rectal cancers. We want to make sure that providers are also focusing on the anus. The purpose of the DARE is to feel for things like hard lumps that might indicate the presence of cancer, but you can’t feel pre-cancers.
I published the first paper showing that the vaccine worked to prevent anal HPV. That’s actually what got the vaccine approved for boys. The vaccine is the best long-term answer: if everyone who fell into current vaccine categories got the vaccine, anal cancer and cervical cancer would be a thing of the past. But it would take decades for that. Anal cancers develop even later than cervical cancers because it takes more years to go from HPV infection to cancer.
Everybody who can get vaccinated, should get the vaccine. The issue though, is there are a lot of people who haven’t gotten the vaccine yet or are too old to get vaccinated. This group needs screening on top of vaccination.
I think that the answer to that varies a lot according to the demographic. Quite a high proportion of my patients are gay men and while there’s still some stigma in that population, on the whole it’s not as remarkable as with some of the other groups that I see in the clinic. For instance, I have quite a few female patients with anal cancer, and they often tell me how difficult it is to talk about the disease to their family and friends.
HPV is stigmatized, cancer is stigmatized, and we don’t like to talk about the anus at all. It’s like the triple whammy. I often refer my patients to the Anal Cancer Foundation which can provide additional emotional support.
HPV Awareness Day is March 4th. The primary message is that HPV is very common, and we’re all affected by it. If you haven’t had it, you know someone who has. We want to make it part of normal conversation and encourage vaccination amongst anyone who is eligible and screening for anyone who is eligible for that.
The theme of the campaign is “One less worry.” One of the things that we emphasize in the campaigns is that we actually do have a message of hope here. We have everything we need right now to make cervical cancer and anal cancer a memory. Not immediately, but for the next generation.

Three organizations—ACS, ACOG, and HRSA—have each recently endorsed new guidelines for cervical cancer screening. All of them discuss screening with self collected samples.
Research suggests that only one dose of the HPV vaccine may be effective enough to prevent HPV-related disease, including cancer.

Australia has been a leader in cervical cancer prevention for decades and is now close to eliminating the disease.

The American Cancer Society (ACS) released new recommendations for cervical cancer screening that focus on HPV testing and approve the use of self-collected samples. The recommendations also clarify the age at which screening should start and stop.
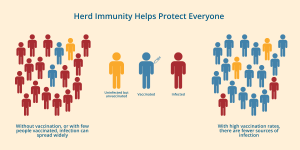
We’ve known for years that the HPV vaccine works. Now new research shows that widespread vaccination even protects those who haven’t gotten the shot. This study proves that it is possible to reach herd immunity for HPV.

The FDA just approved the Teal Wand, a self-collection device for HPV testing that does not require a speculum exam or even a trip to the doctor’s office. People can collect their own sample at home and send it to a lab for analysis.
ASHA believes that all people have the right to the information and services that will help them to have optimum sexual health. We envision a time when stigma is no longer associated with sexual health and our nation is united in its belief that sexuality is a normal, healthy, and positive aspect of human life.
ABOUT
GET INVOLVED
ASHA WEBSITES
GET HELP
© 2026 American Sexual Health Association
We need to know if we can keep you company during this visit. We are useful for making this site work.
We use cookies to enhance your browsing experience. You can choose which cookies you want to accept.
Necessary cookies help make a website usable by enabling basic functions like page navigation and access to secure areas. The website cannot function properly without these cookies.
| Cookie | Provider | Purpose | Expiry |
|---|---|---|---|
digiconsent | This website | Stores your cookie consent preferences. | 1 year |
wordpress_logged_in_* | WordPress | Identifies logged-in users and their authentication details. | 14 days / Session |
wordpress_sec_* | WordPress | Stores authentication details for secure areas. | 14 days / Session |
wp-settings-* | WordPress | Stores user interface customization preferences. | 1 year |
wp-settings-time-* | WordPress | Stores the time when wp-settings cookie was set. | 1 year |
Analytics cookies help us understand how visitors interact with our website by collecting and reporting information anonymously. This helps us improve our website.
| Cookie | Provider | Purpose | Expiry |
|---|---|---|---|
_ga | Registers a unique ID to generate statistical data on website usage. | 2 years | |
_ga_* | Used by Google Analytics to store and count pageviews. | 2 years |
Marketing cookies are used to track visitors across websites. The intention is to display ads that are relevant and engaging for the individual user.
Functional cookies enable the website to provide enhanced functionality and personalization. They may be set by us or by third party providers.