
Mpox Passed on Without Symptoms? New Research Shows It’s Possible
Is mpox passed on without symptoms? In a new study of more than 8,000 men, about 1% of the men tested positive despite never having had symptoms.
Doxy PEP—or doxycycline post-exposure prophylaxis—is a sexual health strategy that involves taking an oral antibiotic after condomless sex to prevent chlamydia, gonorrhea, and syphilis.
This strategy comes at a time when bacterial STIs are on the rise. Recently released data from the CDC showed there were 2.5 million cases of chlamydia, gonorrhea, and syphilis reported in the United States in 2022. Cases of chlamydia and gonorrhea—the two most common reportable STIs—have remained high for many years, and syphilis cases have skyrocketed recently. The number of primary and secondary syphilis infections in 2022 was 80% higher than in 2018.
Doxy PEP is the first new prevention method for bacterial STIs, and many experts believe it will be an important tool in our fight against this epidemic.
Doxy PEP is the strategy of taking the antibiotic doxycycline after condomless oral or anal sex to prevent chlamydia, gonorrhea, or syphilis.
Doxy PEP is intended for adult men who have sex with men and transgender women who have sex with men especially those who have had an STI in the last year. Health care providers may also suggest it to people in this community who have more than one partner.
Some providers might offer doxy PEP to cisgender men who have sex with women if they’ve had condomless sex with more than one partner, especially if they’ve had a bacterial STI like syphilis in the past year. Research with this group is still ongoing.
So far, research has not found doxy PEP to be effective in preventing STIs in cisgender women who have penis-in-vagina sex. More research is being done on this and other populations like adolescents.
You need a prescription for doxy PEP. You can talk to your health care provider or go to a sexual health clinic like those that offer STI testing. Because you have to take doxy PEP quickly after having condomless sex, it’s a good idea to talk to your health care provider about this before you need it.
People using doxy PEP take 200 mg of doxycycline (usually two 100 mg pills) within 72 hours of condomless sex though sooner is better. Doxy PEP can be used every time you have condomless sex, but you shouldn’t take more than 200 mg of doxycycline in a 24-hour period.
Doxycycline is typically inexpensive and usually covered by insurance. Some places may give out doxy PEP for free.
Doxycycline is a common antibiotic that many of us have taken for other infections. Like other antibiotics, it may upset your stomach. Take it with lots of water and try not to lie down for half an hour. Doxycycline may also make you more sensitive to the sun so you should try to avoid prolonged exposure while taking it.
Some people may have more serious reactions. Talk to a health care provider if you have other symptoms—like a bad headache or blurred vision—after taking it.
We have been told over the years that overuse of antibiotics is a problem because it can lead to antibiotic-resistant bacteria (infections that don’t respond to the drugs we have to treat them). There has been some research that doxy PEP might already be contributing to the rise of antibiotic-resistant bacteria. Public health experts still support the use of doxy PEP for people with a higher chance of exposure to STIs. But they do say we need to watch this closely.
Gonorrhea is one of the bacteria that has become resistant to some antibiotics. In fact, about 25% of strains of gonorrhea are resistant to doxycycline. This may be why doxy PEP doesn’t work as well against gonorrhea as it does against chlamydia and syphilis.
Doxy PEP only protects against bacterial STIs. It does not protect against viruses like MPox, HIV, or herpes. The best protection against MPox is the vaccine. If you think you are at risk for HIV, talk to your health care provider about Post-Exposure Prophylaxis (PEP) and Pre-Exposure Prophylaxis (PREP).
Yes. It’s important to keep up with STI screenings and to get checked if you have any symptoms. The CDC recommends that MSM be tested for chlamydia, gonorrhea, and syphilis at least annually and more often (every 3 to 6 months) if you are at increased risk because of HIV infection or multiple partners. Talk to your health care provider about how often you should be screened.
On this episode of the Sex+Health podcast we talk with Jaylan Daniels, who tells us all about doxy PEP and why he chose to include it as part of his health care regimen.
Download our printable fact sheet on doxy PEP, covering who can benefit from taking doxy PEP, how its used, side effects, concerns about antibiotic resistance, and STI testing.

Is mpox passed on without symptoms? In a new study of more than 8,000 men, about 1% of the men tested positive despite never having had symptoms.

New data shows that cases of bacterial STIs have dropped dramatically in San Francisco. Public health officials in the city believe doxy PEP has helped drive these declines.

A new report shows that fewer women are getting prenatal care. That means too many patients are missing the chance to prevent congenital syphilis.

Condoms. All sorts of shapes, sizes, colors (even glow-in-the-dark). Ribbed or plain. Lubed or not. Latex or plastic. ASHA’s Fred Wyand shares his thoughts on this reliable way to prevent STIs and pregnancy.
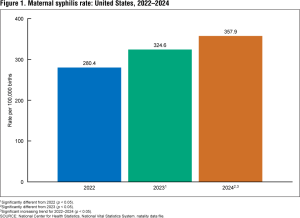
Syphilis rates in pregnant women went up 222% percent between 2016 and 2022 and another 28% between 2022 and 2024. Too many pregnant women are not being screened.

Currently, condoms are the only widely available, proven method for preventing pregnancy and reducing transmission of HIV and other sexually transmitted infections (STIs) during sex. Condoms work.

Three organizations—ACS, ACOG, and HRSA—have each recently endorsed new guidelines for cervical cancer screening. All of them discuss screening with self collected samples.
Research suggests that only one dose of the HPV vaccine may be effective enough to prevent HPV-related disease, including cancer.
ASHA believes that all people have the right to the information and services that will help them to have optimum sexual health. We envision a time when stigma is no longer associated with sexual health and our nation is united in its belief that sexuality is a normal, healthy, and positive aspect of human life.
ABOUT
GET INVOLVED
ASHA WEBSITES
GET HELP
© 2026 American Sexual Health Association
We need to know if we can keep you company during this visit. We are useful for making this site work.
We use cookies to enhance your browsing experience. You can choose which cookies you want to accept.
Necessary cookies help make a website usable by enabling basic functions like page navigation and access to secure areas. The website cannot function properly without these cookies.
| Cookie | Provider | Purpose | Expiry |
|---|---|---|---|
digiconsent | This website | Stores your cookie consent preferences. | 1 year |
wordpress_logged_in_* | WordPress | Identifies logged-in users and their authentication details. | 14 days / Session |
wordpress_sec_* | WordPress | Stores authentication details for secure areas. | 14 days / Session |
wp-settings-* | WordPress | Stores user interface customization preferences. | 1 year |
wp-settings-time-* | WordPress | Stores the time when wp-settings cookie was set. | 1 year |
Analytics cookies help us understand how visitors interact with our website by collecting and reporting information anonymously. This helps us improve our website.
| Cookie | Provider | Purpose | Expiry |
|---|---|---|---|
_ga | Registers a unique ID to generate statistical data on website usage. | 2 years | |
_ga_* | Used by Google Analytics to store and count pageviews. | 2 years |
Marketing cookies are used to track visitors across websites. The intention is to display ads that are relevant and engaging for the individual user.
Functional cookies enable the website to provide enhanced functionality and personalization. They may be set by us or by third party providers.