
HPV Screening with Self Collection Endorsed by Three Organizations
Three organizations—ACS, ACOG, and HRSA—have each recently endorsed new guidelines for cervical cancer screening. All of them discuss screening with self collected samples.

A new study revealed a disturbing trend in health knowledge; fewer people seem to understand the connection between HPV and certain types of cancer including cervical, oral, anal, and penile cancers.
Human papilloma virus, or HPV, is a very common STI. About 79 million people in this country are thought to have an active HPV infection at any given time, and nearly all sexually active people will contract it at some point in their lives. In most cases, the virus is harmless and has no symptoms. The body clears most HPV infections naturally, but certain high-risk types can lead to cancer.
According to this new study, however, many adults are not aware of this link. Researchers analyzed data from the Health Information National Trends Study (HINTS) between 2014 to 2020. HINTS collects data from a nationally representative sample of adults in the United States. This analysis included 10,933 participants. All participants were asked if they’d ever heard of HPV. Those who said they had were then asked, “Do you think HPV can cause anal, cervical, oral, and penile cancers?”
The results, which were presented at the annual meeting of the American Association for Cancer Research, were disturbing. Only 70% of participants had ever heard of HPV. Of those, only 70% knew it was linked to cervical cancer, which is a 7.4% drop when compared to 2014 participants. While the decline in knowledge was less steep for other HPV-related cancers, awareness was low: only 29% knew HPV was linked to oral cancer, 28% to penile cancer, and 27% to anal cancer.
The study doesn’t tell us why HPV knowledge has dropped though some public experts theorized that the focus on the pandemic pulled attention away from many, if not all, other public health issues. These results are important because previous research has found that awareness of the link between HPV and cancer increases vaccine uptake.
There are approximately 37,300 cases of HPV-related cancers each year in the United States including 11,100 cases of cervical cancer; 14,800 cases of throat cancer; 6,900 cases of anal cancer; 2,900 cases of vulva cancer; 900 cases of penile cancer; and 700 cases of vagina cancer. The CDC estimates that 90% of these cancers could be prevented with vaccination.
The agency recommends that all young people get the vaccine as part for routine vaccinations for 11-12 year-olds. Research shows that the vaccine produces a stronger immune response when given during the preteen years, and fewer shots are required. Also, the vaccine is designed to prevent infection with HPV, so vaccination is recommended at a young age—before kids are exposed to the virus.
Still, vaccination rates for HPV lag behind other routine vaccinations. Misinformation about vaccines has been swirling around for decades, and anti-vaccine sentiment seems to be on the rise since the introduction of the Covid-19 vaccines. HPV vaccines have been the subject of misinformation and misunderstanding about their efficacy and safety as well as myths around sexuality that suggest young people will increase their sexual activity if vaccinated.
The HPV vaccine is safe. Over 120 million doses of the HPV vaccine have been distributed since the vaccine was licensed, and data has shown it to be safe and well tolerated. While some parents have expressed a concern that vaccinating their children against HPV will lead to increased sexual behavior, many studies have shown this not to be the case.
Public health experts have been trying to move away from discussing HPV vaccination in relation to STI prevention and emphasizing instead that the vaccine prevents cancer. This new study, however, shows that such awareness is still lacking.

Three organizations—ACS, ACOG, and HRSA—have each recently endorsed new guidelines for cervical cancer screening. All of them discuss screening with self collected samples.
Research suggests that only one dose of the HPV vaccine may be effective enough to prevent HPV-related disease, including cancer.

Australia has been a leader in cervical cancer prevention for decades and is now close to eliminating the disease.

The American Cancer Society (ACS) released new recommendations for cervical cancer screening that focus on HPV testing and approve the use of self-collected samples. The recommendations also clarify the age at which screening should start and stop.
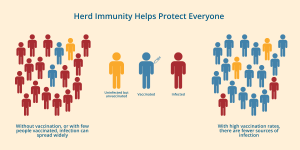
We’ve known for years that the HPV vaccine works. Now new research shows that widespread vaccination even protects those who haven’t gotten the shot. This study proves that it is possible to reach herd immunity for HPV.

The FDA just approved the Teal Wand, a self-collection device for HPV testing that does not require a speculum exam or even a trip to the doctor’s office. People can collect their own sample at home and send it to a lab for analysis.

The results of large-scale study of HPV suggest that one shot of the vaccine may be enough to protect young people from HPV and related issues like cervical cancer.

You have probably heard that HPV can cause cervical cancer. But did you know that it can also cause cancers of the mouth, tongue, and throat?
ASHA believes that all people have the right to the information and services that will help them to have optimum sexual health. We envision a time when stigma is no longer associated with sexual health and our nation is united in its belief that sexuality is a normal, healthy, and positive aspect of human life.
ABOUT
GET INVOLVED
ASHA WEBSITES
GET HELP
© 2026 American Sexual Health Association
We need to know if we can keep you company during this visit. We are useful for making this site work.
We use cookies to enhance your browsing experience. You can choose which cookies you want to accept.
Necessary cookies help make a website usable by enabling basic functions like page navigation and access to secure areas. The website cannot function properly without these cookies.
| Cookie | Provider | Purpose | Expiry |
|---|---|---|---|
digiconsent | This website | Stores your cookie consent preferences. | 1 year |
wordpress_logged_in_* | WordPress | Identifies logged-in users and their authentication details. | 14 days / Session |
wordpress_sec_* | WordPress | Stores authentication details for secure areas. | 14 days / Session |
wp-settings-* | WordPress | Stores user interface customization preferences. | 1 year |
wp-settings-time-* | WordPress | Stores the time when wp-settings cookie was set. | 1 year |
Analytics cookies help us understand how visitors interact with our website by collecting and reporting information anonymously. This helps us improve our website.
| Cookie | Provider | Purpose | Expiry |
|---|---|---|---|
_ga | Registers a unique ID to generate statistical data on website usage. | 2 years | |
_ga_* | Used by Google Analytics to store and count pageviews. | 2 years |
Marketing cookies are used to track visitors across websites. The intention is to display ads that are relevant and engaging for the individual user.
Functional cookies enable the website to provide enhanced functionality and personalization. They may be set by us or by third party providers.