
HPV Screening with Self Collection Endorsed by Three Organizations
Three organizations—ACS, ACOG, and HRSA—have each recently endorsed new guidelines for cervical cancer screening. All of them discuss screening with self collected samples.
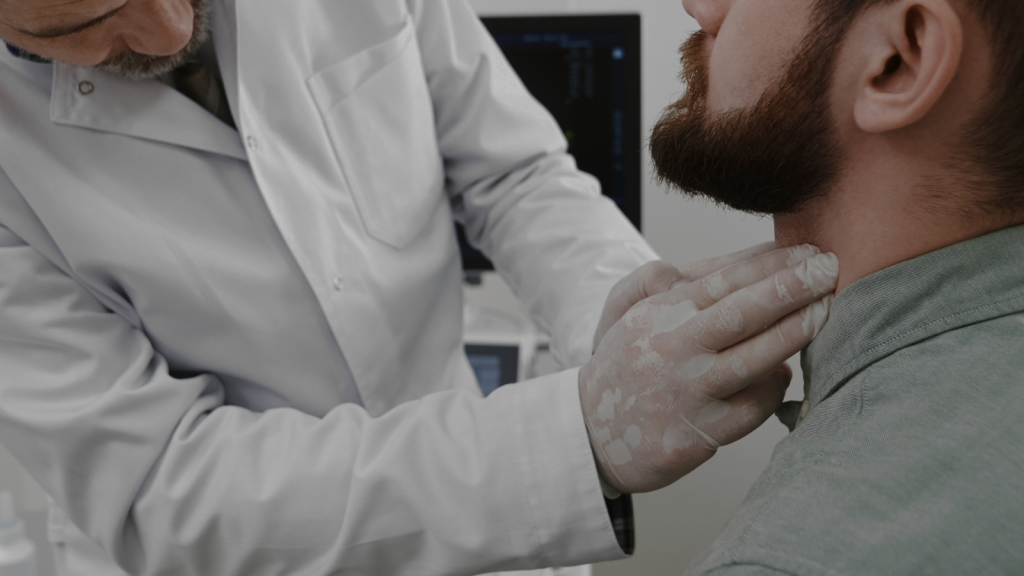
Michael Moore, MD, is the Chief of the Division of Head and Neck Surgery at the Indiana University School of Medicine Department of Otolaryngology. He specializes in cancer removal and reconstructive surgery and works as a part of multidisciplinary team that manages treatment for head and neck cancer patients. Dr. Moore has also served as the Chair of the Cancer Prevention Service of the American Head and Neck Society (AHNS), a member of the American Cancer Society HPV Vaccination Roundtable, and as President of the Board of the Head and Neck Cancer Alliance.
ASHA recently sat down with Dr. Moore to ask about head and neck cancers caused by HPV.
Head and neck cancer is just a general term to describe any malignant tumors that start anywhere above the collarbone and below the brain. They can be everything from skin cancers to mouth and throat cancers to those that affect the back of the throat or voice box. They also include salivary cancer and thyroid cancers.
The primary risk factors for head and neck cancer historically were tobacco and alcohol use because they are carcinogens that affected the areas they came in contact with like the lining of the mouth and throat. Those have been slowly going down over the years because education and tobacco taxes means there’s less and less smoking and the result is less and less tobacco-related cancers which is great.
The only area where incidence of head and neck cancer is going up is in what we call oropharyngeal cancers. These are usually at the back of the throat and are primarily due to HPV infection.
No. These cancers usually occur at the base of the tongue or in the tissue around the tonsils. If you’re looking at the back of your mouth, it’s kind of around the corner where you can’t see. This tissue has little pits in them that filter stuff as part of your immune system and those pits can act as a reservoir. When you get a viral infection, it can hang out at the bottom of those pits which makes that area more susceptible for cancers.
Yes. HPV 16—which is also the cause of most cervical cancer—is the primary driver for head and neck cancer related to HPV. About 90% of the oropharynx cancers are related to this type.
We think so and there has been some research to support this. We know that it protects against high-risk HPV infection which is great. The challenge in determining how well the vaccine works is that there is a long latency period between infection and oropharyngeal cancer. Maybe even 20 or 30 years.
And we don’t have any tests for precancerous legions like we do for cervical cancer. The vaccine hasn’t been around for that long. Most of the people who get oropharyngeal cancers are in their 50s and probably got exposed when they were adolescents or young adults. It’s going to take some years before we’re able to show that the vaccine is working on a large scale.
Yes. The protective effect of reducing persistent infection is important, and I think studies will ultimately find that it reduces the risk of head and neck cancers as well. I’m not a population person but I also think vaccinating more people will have a kind of overall protective effect. If infection rates overall go down that will have downstream benefits for cancer development.
There are no screening tests yet. There are some new blood tests that look for what’s called the HPV cell free DNA. These aren’t screening tests; they’re used to get more information when we’re planning cancer treatment. It’s possible that they will advance at some point to something similar to a PSA test for prostate cancers but not yet.
There are also not always symptoms. In other types of head and neck cancer, like those caused by tobacco, a person might have difficulty swallowing or persistent throat pain because the primary tumor is aggressive. But with cancer of the oropharynx caused by HIV, the primary tumor is usually very small. Sometimes it’s so small, that I can’t even see it when I look down someone’s throat.
The most common presenting symptom for a person with HPV-related throat cancer is a neck mass, like a lump in the neck. That’s actually a lymph node metastasis already which means the cancer has already spread. I’m an oncologist so I see people who have been diagnosed with cancer, when they get to me their main symptoms other than the lymph node may be a change in their voice, difficulty swallowing, or throat pain, often only on one side. Sometimes they have pain in their ear that is actually referred pain from their throat, and they may be coughing up blood.
A lot of it depends on the extent of the tumor and where it is. There are two ways to approach it. One is to start with surgery and take out the primary tumor and possibly some lymph nodes. And then depending on how early the cancer was caught we might just monitor it closely or we might decide to do radiation and/or chemotherapy to reduce the chance that there’s some microscopic cancer that would grow back. There’s also the non-surgical option that just uses radiation for early disease and chemotherapy for advanced disease.
These are some of the longest conversations I have with my patients because they’re very different. With surgery you may have more upfront side effects like pain and trouble swallowing until your throat is healed. With higher doses of radiation, you may get dryness of the mouth or damage to the taste bud. These are the factors patients have to weigh.
As long as it’s not spread to other parts of the body, survival rates for HPV-related head and neck cancer can be between 80% and 90% or even higher. This is much better than survival rates for head and neck cancers caused by smoking.
Most likely yes. There have been studies that show that an increased number of oral sex partners and early sexual debut are risk factors for developing HPV-related oropharynx cancer. But I think there’s a lot that we still don’t know.
It’s about four to one, men to women as far as who gets oropharynx cancer, but men who have sex with men are not necessarily at dramatically increased risk. An increased viral concentration of HPV in vaginal secretions might explain why the heterosexual population can be affected significantly by this. The immune system might also play an underlying role, but we don’t know all of it yet.
They’ve usually heard of the virus. Most of them have heard of it in regards to cervical cancer but many of them have not heard of it in the context of throat cancer.
With head and neck cancers there is stigma to begin with because many people think it’s related to tobacco use and patients think it was their fault because they smoked. I do think there’s also some stigma around the idea of promiscuity because we still have a lot of societal stigma around sex unfortunately.
I think people are also worried when they’re talking to their spouse, I try to stress that it’s impossible to say where HPV came from, or which partner it came from.
I also try to stress to my patients that the vast majority of adults have been exposed to HPV and that throat cancer is now the most common HPV-related cancer in America. It is close to two times as common as cervical cancer now.
The biggest thing is that many cases of cervical cancer are caught in the precancerous stage. The vaccine is also good but there is a bit of a lag before we’ll see that. For head and neck cancer it’s really a combination of not having good screening tests, males getting the vaccine less frequently, and a longer latent period before cancers develop. So even if vaccination in the younger groups is happening, there is a group of people over the next 20 or 30 years who will be developing these cancers because they have already gotten HPV.
I think our Holy Grail for reducing these cancers is going to be finding a screening test that can be widely used.
Download the fact sheet to get fast facts about HPV-related head and neck cancer. Learn about the connection between HPV infection and cancers of the back of the throat, the differences between rates of this type of cancer in men and women, and how you can protect yourself and prevent cancer with HPV vaccination.

Three organizations—ACS, ACOG, and HRSA—have each recently endorsed new guidelines for cervical cancer screening. All of them discuss screening with self collected samples.
Research suggests that only one dose of the HPV vaccine may be effective enough to prevent HPV-related disease, including cancer.

Australia has been a leader in cervical cancer prevention for decades and is now close to eliminating the disease.

The American Cancer Society (ACS) released new recommendations for cervical cancer screening that focus on HPV testing and approve the use of self-collected samples. The recommendations also clarify the age at which screening should start and stop.
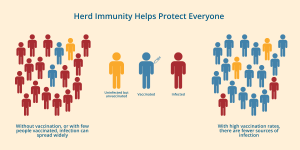
We’ve known for years that the HPV vaccine works. Now new research shows that widespread vaccination even protects those who haven’t gotten the shot. This study proves that it is possible to reach herd immunity for HPV.

The FDA just approved the Teal Wand, a self-collection device for HPV testing that does not require a speculum exam or even a trip to the doctor’s office. People can collect their own sample at home and send it to a lab for analysis.

The results of large-scale study of HPV suggest that one shot of the vaccine may be enough to protect young people from HPV and related issues like cervical cancer.

You have probably heard that HPV can cause cervical cancer. But did you know that it can also cause cancers of the mouth, tongue, and throat?
ASHA believes that all people have the right to the information and services that will help them to have optimum sexual health. We envision a time when stigma is no longer associated with sexual health and our nation is united in its belief that sexuality is a normal, healthy, and positive aspect of human life.
ABOUT
GET INVOLVED
ASHA WEBSITES
GET HELP
© 2026 American Sexual Health Association
We need to know if we can keep you company during this visit. We are useful for making this site work.
We use cookies to enhance your browsing experience. You can choose which cookies you want to accept.
Necessary cookies help make a website usable by enabling basic functions like page navigation and access to secure areas. The website cannot function properly without these cookies.
| Cookie | Provider | Purpose | Expiry |
|---|---|---|---|
digiconsent | This website | Stores your cookie consent preferences. | 1 year |
wordpress_logged_in_* | WordPress | Identifies logged-in users and their authentication details. | 14 days / Session |
wordpress_sec_* | WordPress | Stores authentication details for secure areas. | 14 days / Session |
wp-settings-* | WordPress | Stores user interface customization preferences. | 1 year |
wp-settings-time-* | WordPress | Stores the time when wp-settings cookie was set. | 1 year |
Analytics cookies help us understand how visitors interact with our website by collecting and reporting information anonymously. This helps us improve our website.
| Cookie | Provider | Purpose | Expiry |
|---|---|---|---|
_ga | Registers a unique ID to generate statistical data on website usage. | 2 years | |
_ga_* | Used by Google Analytics to store and count pageviews. | 2 years |
Marketing cookies are used to track visitors across websites. The intention is to display ads that are relevant and engaging for the individual user.
Functional cookies enable the website to provide enhanced functionality and personalization. They may be set by us or by third party providers.